| Journal of Food Bioactives, ISSN 2637-8752 print, 2637-8779 online |
| Journal website www.isnff-jfb.com |
Original Research
Volume 10, June 2020, pages 64-69
Evaluation of the hypo-allergenicity effect of rice and wheat hydrolysates: a double-blind randomized clinical trial
Hui-Fang Chiua, You-Cheng Shenb, Yi-Chun Hanc, Kamesh Venkatakrishnanc, Chin-Kun Wangc, *
aDepartment of Chinese Medicine, Taichung Hospital Ministry of Health and Welfare, Taichung-40301, Taiwan, ROC
bSchool of Health Diet and Industry Management, Chung Shan Medical University, 110, Sec. 1, Jianguo North Road, Taichung City, Taiwan, ROC
cSchool of Nutrition, Chung Shan Medical University, 110, Sec. 1, Jianguo North Road, Taichung City-40201, Taiwan, ROC
*Corresponding author: Chin-Kun Wang, School of Nutrition, Chung Shan Medical University, 110, Sec. 1, Jianguo North Road, Taichung City-40201, Taiwan, ROC. Tel: +886 4 22653397; Fax: +886 4 22654529; E-mail: wck@csmu.edu.tw
DOI: 10.31665/JFB.2020.10228
Received: January 13, 2020
Revised received & accepted: June 24, 2020
| Abstract | ▴Top |
This study was conducted to evaluate and compare the anti-allergenicity effect of rice and wheat hydrolysates in food allergic subjects. Totally fifty food allergic subjects (confirmed by allergic score) were recruited and divided into 2 groups as rice hydrolysate (RH; n = 40) and wheat hydrolysate (WH; n = 10) and asked to take either rice or wheat hydrolysate formula for 4 weeks. After 4 weeks of intervention with RH, the levels of the allergic score, allergic inflammatory markers like eosinophil count (EC) and eosinophil cation protein (ECP), as well as in total IgE, total nasal symptom score (TNSS) were significantly reduced as compared to the baseline. However, WH supplemented (4 weeks) group showed a mild increase in total IgE, EC (but no change in inflammatory markers, ECP, TNSS) along with decreased SCORAD (SCORing Atopic Dermatitis) index as compared to the baseline. Overall, the subjects that consumed the RH formula for 4 weeks showed a marked decrease in the allergic parameters except for the SCORAD index and thus endorsing its potent anti-allergenicity property better than WH (which indeed aggravated EC, IgE levels). Therefore, RH might be recommended with other standard anti-allergic drugs to delay or suppress allergic symptoms and its related allergic responses.
Keywords: Rice hydrolysate; Wheat hydrolysate; Allergic index; TNSS; SCORAD skin test
| 1. Introduction | ▴Top |
Food allergy (FA) is a condition in which some food components (particularly protein) are recognized as foreign materials by host immune system and subsequently elicit various immunological responses (Cianferoni and Spergel, 2009). Several studies have reported that 8% of children and 2% of the adult have some sort of food allergy and the prevalence rate (especially in children) is increasing day-by-day and thus has a direct impact on global and family economic status (Sicherer and Sampson, 2018; Cianferoni and Spergel, 2009). Moreover, FA might also result in severe morbidity and rarely mortality and thus considerably reduces the quality of life as it has a strong correlation with many allergic manifestations including asthma, atopic dermatitis or eczema (Nurmatov et al., 2017; Canani et al., 2017). The major classification of FA is IgE mediated, non-IgE mediated (cell-mediated) and mixed IgE and cell-mediated FA. The common food allergens include cow’s milk, egg, fish, shellfish, peanuts, tree nuts (hazelnut, walnut, cashew, pistachio, Brazil nut, almond, pecans, macadamia, chestnuts), soy, wheat gluten of which the proteins are considered as the major culprit for FA (Cianferoni and Spergel, 2009). Food allergies are mostly determined by various test and their related symptoms including bloating, diarrhea, nausea/vomiting, enterocolitis (GI problems), rhinitis, wheezing, dry cough, asthma (nasal or respiratory problems) and atopic dermatitis/eczema (dermal problems) (Spergel and Sharma, 2016; Sicherer and Sampson, 2010).
Currently, avoiding allergic food is the only possible option to manage food allergy. Nevertheless, accidental exposure of food allergens could trigger an immune response and end up in fatal anaphylaxis or hypersensitivity reaction (Muraro et al., 2014). Hence, food allergic individuals are recommended to carry adrenalin auto-injector to manage anaphylaxis for only a short time until they reach a hospital or clinics (Sicherer and Sampson, 2010; Sampson, 2003). Moreover, allergen immunotherapy (AIT: administration of silver) is also used to manage food allergy and its associated symptoms, but effective only against IgE mediated food allergy (Nurmatov et al., 2017). Hence, the need for a potent anti-allergenic agent to manage food allergic reactions is of an enormous demand. Previously, many researchers have indicated that both rice and wheat hydrolysate (protein) formula displayed some positive result against various abnormal or pathological conditions as well as to combat various food allergic conditions (hypoallergic formula-especially in kids/infants). Also, they are inexpensive, have good acceptability (palatability) and high nutrient value (Bocquet et al., 2019; Sicherer and Sampson, 2018; Vandenplas et al., 2014; Fiocchi et al., 2006). Hence, we hypothesize that intervention with rice hydrolysate (RH) or wheat hydrolysate (WH) might decrease or eliminate food allergic reaction and its related symptoms in both adults and children.
| 2. Materials and methods | ▴Top |
2.1. Rice and wheat hydrolysate formula
The commercial rice and wheat hydrolysate formula were supplied by Quaker (Standard Food Corporation), Taipei, Taiwan. The rice hydrolysate (RH) mainly comprised of carbohydrates (14.6 g), protein (1.2 g especially essential amino acids i.e lysine, phenylalanine, and threonine-protein/peptide hydrolysate), fat (0.9 g), sodium, calcium, and magnesium equivalent to 71 kCal. While the composition of wheat hydrolysate (WH) included carbohydrates (14.6 g), protein (1.9 g with amino acids like valine, leucine), fat (0.5 g), sodium, calcium, and magnesium equivalent to 71 kCal. Both rice and wheat formula are packed in a similar package and have similar color and flavor.
2.2. Subjects enrollment
This clinical trial was conducted at Chung Shan Medical University Hospital, Taiwan and was approved by the institutional ethical review board (CS05010). In the beginning, seventy-two food allergic subjects aged between 5 to 75 years (confirmed by an allergic score based on allergic symptoms) were enrolled into this trial through posters (hospital and public places) and newspaper advertisement. The major inclusion criteria as follows: must be allergic patient (confirmed by an allergic score based on allergic symptoms- questionnaires) and should be positive with food-specific IgE and SCORAD skin test and should not be under any medications like antihistamine or corticosteroid. Whereas, the exclusion criteria include severe allergic reaction, history of nasal reconstruction or surgery, medical illness or chronic renal or hepatic disorders, pregnant or nursing women and intake of dietary supplements. All the subjects or their parents/guardian must sign the consent before enrolling into this trial.
2.3. Study design
Based on inclusion and exclusion criteria (as mentioned above), only 50 subjects were eligible and enrolled into this clinical trial and divided into 2 groups as rice hydrolysate (RH; n = 40) and wheat hydrolysate (WH; n = 10). Each subject was requested to take either RH or WH formula for 4 weeks, by replacing one meal every day. Subjects could withdraw from this trial at any point of time. All the subjects were asked to visit the hospital every 2 weeks, to check various allergic symptoms (questionnaires) and allergic conditions as well as to collect the samples (WH or RH). Blood samples were collected only at baseline (0 weeks) and 4th week (end of the intervention) and serum samples were separated to check various inflammatory allergic parameters. In this work we opted not to use any positive controls.
2.4. Measurement of inflammatory allergic markers
2.4.1. Eosinophil count, Eosinophil cation protein (ECP) and total serum IgE
The whole blood sample was used to measure the eosinophil count (EC) using SYSMEX SE-900 automated hematological analyzer. While, the levels of serum ECP and total IgE were determined by commercial fluorescence enzyme-linked immunosorbent assay (ELISA anti-ECP and Anti-IgE-Immuno assay kit) using immunoCAP and UniCAP 100 system (Pharmacia, Union City, NJ, USA) based on manufacturers protocol.
2.5. Overall patient allergic score (allergy index)
The allergic score was evaluated based on various allergic symptoms (questionnaires) including the itchy nose, rhinorrhea (runny nose), obstructed or congested nose, sneezing, itchy watery eyes, dry cough, hives, eczema, itchy skin, swelling, indigestion, constipation, diarrhea, fatigue (on daily basis). Moreover, specific condition for different symptoms were also checked like seasonal allergic symptoms (summer, spring, autumn or winter), outdoor or perennial allergic symptoms (things/materials/animal-related allergic symptoms-latex, vacuum cleaner, handling animals-cat/dogs/dust mites & cockroaches), previous IgE or skin test results (allergic history), as well as family allergic details were noted. Each symptom carried different points (total point ranges from 0 to 16). If the total point was less than 7 , the subject was considered as being not allergic; if between 8 and 12 may be allergic (confirmed with further test like physical or blood/skin test); if the total allergic point was greater than 12, the subject was considered allergic. The overall allergic score was calculated by the method of Annesi-Maesano and his colleagues (2002) with slight modification (however no standard method to assess the allergic score).
2.6. TNSS score (questionnaires)
The repeatability of the total nasal symptom score (TNSS) is the sum of nasal symptom score, which was checked to assess the condition of nasal allergic symptoms. TNSS was measured as four-point rating scale which included TNSS frequency score (0–4 for each symptom) and TNSS degree of distress score (0–4 for each symptom) based on various questionnaires which comprised various allergic symptoms like nasal itchiness, nasal obstruction, rhinorrhea and sneezing as indicated previously by Jung et al. (2011a).
2.7. SCORAD (SCORing Atopic Dermatitis) Skin test index
The SCORAD index was assessed to check the severity of allergy especially related to atopic dermatitis (AD), which was developed by the European task force on atopic dermatitis (1993) and for this study, we followed Chung (2010) method for determining SCORAD. Briefly, the area of skin lesions was determined and followed by checking for erythema, crust, edema, excoriation, lichenification, skin dryness and rated from 0 to 3. Also, the degree of itching (pruritis), sleep deprivation (0 to 10) using VAS were measured. Finally, based on the above score SCORAD index (0 to 103) were calculated using the below formula:
2.8. Data analysis
All values are expressed as mean ± standard error mean (SEM). The significant difference between the baseline (0 week) Vs 2nd week Vs 4th week (each experimental group: RH or WH) was analyzed using Student paired t-test using SPSS software (IBM, Armonk, NY, USA). A p-value of less than 0.05 was deemed statistically significant.
| 3. Results | ▴Top |
3.1. Baseline characteristics
Table 1 shows the baseline characteristics of all subjects, which included sex, age, EC, ECP, and total IgE levels. A significant difference was noted in the EC and total IgE values at baseline between the RH Vs WH group. The overall allergic score or index is shown in Table 2. As the weeks passed by, the allergic score in the RH group gradually decreased and at the end of the 4th week, the level of the allergic score decreased considerably as compared to the baseline. However, the WH group did not show any significant difference after 4 weeks of intervention with WH.
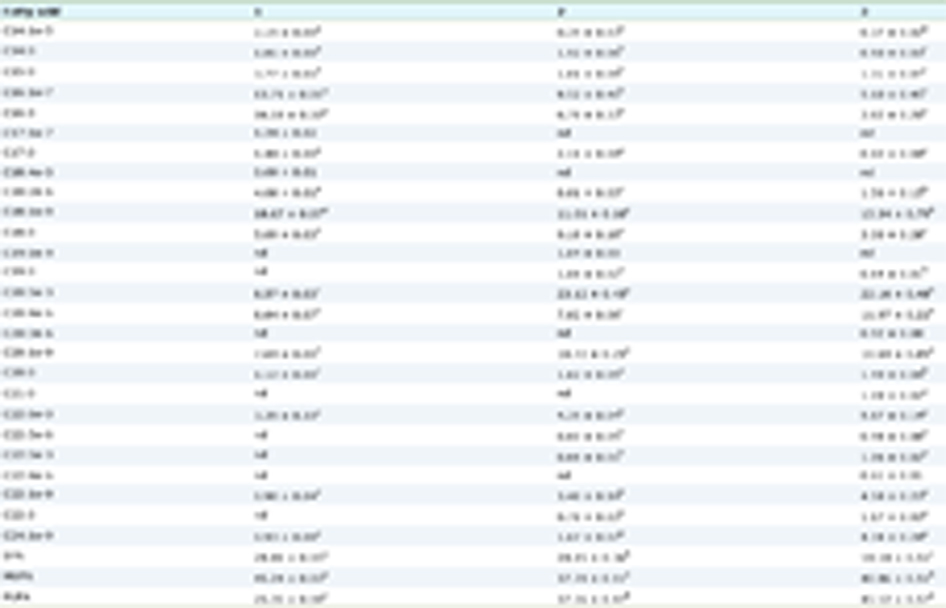 Click to view | Table 1. Shows the baseline characteristics of all subjects |
 Click to view | Table 2. Shows the overall patient allergic score (based on questionnaires) |
3.2. Inflammatory allergic markers
The effect of RH and WH formula on blood inflammatory allergic markers like EC, ECP, and total IgE levels are shown in Table 3. Upon 4 weeks of treatment with RH, the levels of EC and ECP were substantially decreased, without altering total IgE levels as compared to the baseline. Nevertheless, the WH administered allergic subjects showed elevated EC and total IgE values, without altering the ECP level. Both RH and WH showed a different way of interaction with blood inflammatory allergic markers.
 Click to view | Table 3. Shows the blood eosinophil and IgE count |
3.3. TNSS and SCORAD Score
Table 4 shows the TNSS frequency and degree of distress score. Subjects administered with RH for 4 weeks, showed a marked decline in the scores of both TNSS frequency and degree of distress on equivalence with 0 week (baseline). No significant changes were observed in WH intervened subjects. The SCORAD skin score/index of allergic patients was epitomized in table 5. A significant decrease in the SCORAD score was observed in the WH group, but the RH group showed no significant change as compared to baseline.
 Click to view | Table 4. Shows the TNSS frequency and distress score |
 Click to view | Table 5. Shows the SCORAD Skin test scale |
| 4. Discussion | ▴Top |
Both rice (Oryza sativa) and wheat (Triticum aestivum) are common staple foods consumed globally. Also, the hydrolysate (formula) of both rice and wheat have been extensively studied and many researchers have demonstrated that both rice and wheat protein hydrolysates (protein formula) have shown a positive impact on various pathological conditions as well as in treating food allergic conditions (Bocquet et al., 2019; Sicherer and Sampson, 2018; Vandenplas et al., 2014; Fiocchi et al., 2006; D’Auria et al., 2003). Based on the above knowledge, we designed a clinical trial to assess the impact of rice hydrolysate (RH) and wheat hydrolysate (WH) against various food allergic reaction or response and its related symptoms in both adults and children (food allergic subjects) by evaluating various allergic symptoms/markers and index and to compare the results. The outcome of the present trial revealed that intervention with RH (4 weeks) considerably lowered the level of the allergic score, inflammatory allergic markers, and TNSS frequency and degree of distress score as compared to baseline. However, WH did not show any significant changes in any of the allergic parameters except the SCORAD score.
Generally, the impact of food allergy is calculated based on various allergic symptoms, which are represented as an allergic score. During this trial, the levels of overall allergic score or index were evaluated. As compared to the baseline (0 week) the allergic score was significantly reduced upon 4 weeks of intervention with RH. Nonetheless, the subjects that consumed WH did not display any significant difference after 4 weeks of intervention. The inflammatory allergic markers (EC, ECP) play a crucial role in an allergic reaction and hence those markers were evaluated in this study. Eosinophils (major inflammatory cells) is involved in the inflammatory process which is generally triggered by various allergens. Hence, eosinophil count (EC) were assessed to check and predict the severity of allergy (Eguiluz-Gracia et al., 2018; Chen et al., 2006). In addition, ECP is a basic protein released by granules of eosinophil after encountering allergens (pathogens). ECP has been detected in numerous pathological allergic conditions like asthma, rhinitis, atopic dermatitis and found mainly in serum, nasal fluid, sputum or saliva. Therefore, ECP was measured to cross-check the severity of allergic symptoms or manifestation (Kirgezen et al., 2019; Metcalfe et al., 2016). Administration with RH (rich in protein/peptide hydrolysate) for 4 weeks considerably suppressed, the levels of EC and ECP as compared to the baseline. A similar trend was noted in the studies conducted by D’Auria et al., (2003). Moreover, Vandenplas et al. (2014) reported that intervention of hydrolysate formula (especially from rice, soy and cow milk) rich in peptides are the major contributors for anti-allergic properties. Similarly, we hypothesize that the protein/peptide hydrolysate present in RH might be the major contributor for the above results. However, further studies are needed to isolate particular peptide(s) from RH and evaluate its (their) anti-allergic activity.
Moreover, immunoglobulin E (IgE) is the least immunoglobulin, which contributes only 0.01% of total Igs and highly expressed during allergic conditions (Lombard et al., 2015). IgE is secreted by the plasma B cells (basophils) in the gastric tract (endothelial) and respiratory tract (ciliated/goblet cells) after the invasion of allergens. Food specific IgE also acts as an indicator/biomarker of allergic symptoms and food sensitivity (Yunginger et al., 2000). However, few studies have demonstrated that IgE was not altered after food allergy and cannot be used as a diagnostic marker for allergy especially allergic rhinitis (Jung et al., 2011b; Nickeisen et al., 1986). Likewise, our study also revealed no significant changes in IgE levels were observed in the RH or WH group.
The TNSS frequency and degree of distress score were used to indirectly portrait the quality of life (stress), due to allergic reaction as well as the SCORAD skin index which reflects the degree of allergy (Matricardi, 2010). Hence, the author decided to check whether RH or WH improves the quality of life (lower stress and degree of allergy) in allergic subjects by checking both the TNSS score and SCORAD skin index. Subjects supplemented with RH for 4 weeks, showed a marked decline in the TNSS scores (TNSS frequency and degree of distress). Whereas, no changes were noted in WH group. However, the SCORAD skin score/index was substantially decreased in WH group subjects, but the RH group showed no significant change as compared to baseline. The exact reason for the change in SCORAD skin score by WH, need to be further explored in future studies. Overall, RH showed potent anti-allergic property than WH, it might be due to a high level of hydrolysis in RH. Similarly, a randomized, double-blind clinical trial conducted by von Berg et al. (2003), inferred that the degree of hydrolysis of cow milk would modify the nutritive value, which might indirectly involve in the anti-allergenicity property (preventive effect) and thus delay or suppress various allergic symptoms or manifestation. The major limitation of this study is the lack of a control group for comparison. However, this preliminary trial that aimed to just evaluate and compare the anti-allergenicity effect of rice and wheat hydrolysates in food allergic subjects provided a better option for treatment of allergy sufferers. Future studies should fine tune the findings of this study and to also use a positive control group for comparison.
| 5. Conclusion | ▴Top |
Taking together, that allergic subjects supplemented with RH for 4 weeks exhibited a considerably lower allergic parameters like allergic score, inflammatory allergic markers, and TNSS frequency and degree of distress score except for the SCORAD index and thus displayed better anti-allergenic property than WH. However, more studies are needed to confirm the molecular mechanism behind the anti-allergenicity effect of rice hydrolysate, before it could be recommended with other standard anti-allergic agents to delay or suppress various allergic symptoms or manifestation (FA) in adult and child allergic subjects.
Conflict of interest
No conflict of interest to disclose for this trial.
| References | ▴Top |